Lung Cancer: Symptoms, Treatment, and Prevention
Lung cancer is one of the most common and serious types of cancer worldwide. It often develops quietly and may not cause noticeable symptoms until it has reached an advanced stage. Recognizing early signs, learning about treatment options, and taking preventive steps can make a significant difference in outcomes.
Lung cancer begins when abnormal cells in the lungs grow and multiply uncontrollably. When the cancer starts in the lungs, it is known as primary lung cancer. If cancer begins elsewhere in the body and spreads to the lungs, it is called secondary (or metastatic) lung cancer.
In Australia, lung cancer is the leading cause of cancer-related deaths and is the fifth most commonly diagnosed cancer (excluding non-melanoma skin cancers). It accounts for nearly one in five cancer deaths across the country.
There are two main types of lung cancer:
Non-small cell lung cancer (NSCLC)
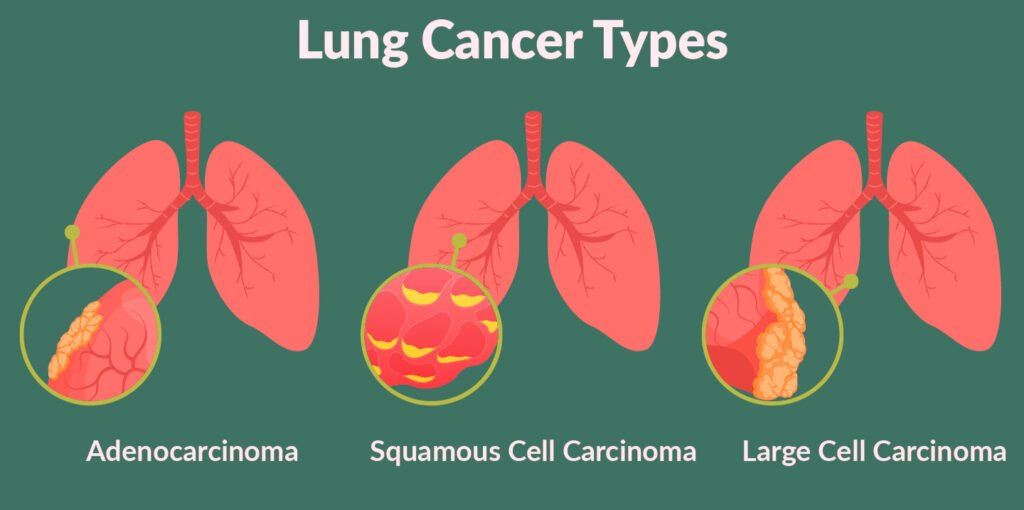
Non-small cell lung cancer is the most common type of lung cancer, accounting for around 85% of cases. There are sub-types of non-small cell lung cancer. The most common are:
- adenocarcinoma – begins in mucus-producing cells and makes up about 40% of lung cancers. While this type of lung cancer is most commonly diagnosed in current or former smokers, it is also the most common lung cancer in non-smokers.
- squamous cell (epidermoid) carcinoma - commonly develops in the larger airways of the lung.
- large cell undifferentiated carcinoma - can appear in any part of the lung and are not clearly squamous cell or adenocarcinoma.
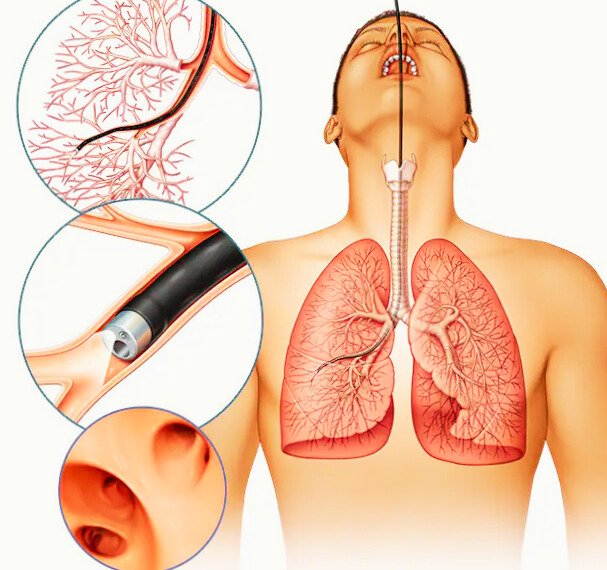
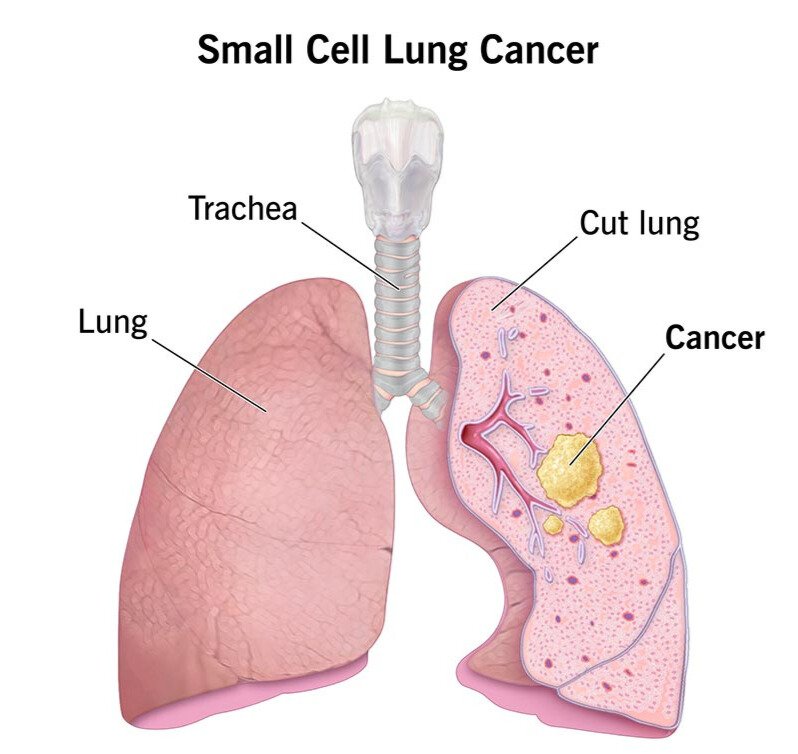
Small cell lung cancer (SCLC)
Small cell lung cancer usually begins in the middle of the lungs and spreads more quickly than non-small cell lung cancer. It accounts for around 15% of lung cancers.
Symptoms
Early lung cancer may not cause any symptoms. When symptoms appear, they can include:
- A new cough or one that worsens over time
- Shortness of breath, even with light activity
- Chest pain, especially when coughing, laughing, or breathing deeply
- Coughing up blood (hemoptysis)
- Unexplained weight loss and loss of appetite
- Persistent fatigue or weakness
- Frequent or recurring lung infections such as pneumonia or bronchitis
- Hoarseness or changes in voice
Causes of lung cancer
Factors that can increase your risk of lung cancer include:
- smoking tobacco
- second-hand (passive) smoking
- exposure to asbestos
- exposure to radon (radioactive gas)
- exposure to occupational substances such as arsenic, cadmium, nickel, diesel fumes and soot
- HIV infection
- family history
- history of lung diseases such as lung fibrosis or emphysema
- older age
Treatment
Treatment depends on the type of lung cancer (small cell or non-small cell) and the stage at diagnosis. Options may include:
- Surgery – Removal of tumors, often using minimally invasive techniques such as video-assisted thoracoscopic surgery (VATS).
- Radiation therapy – High-energy rays, including stereotactic body radiotherapy (SBRT), used to kill cancer cells.
- Chemotherapy – Drugs that destroy cancer cells, sometimes combined with surgery or radiation.
- Targeted therapy – Medicines designed to block specific abnormalities in cancer cells.
- Immunotherapy – Treatments that boost the body’s immune system to fight cancer.
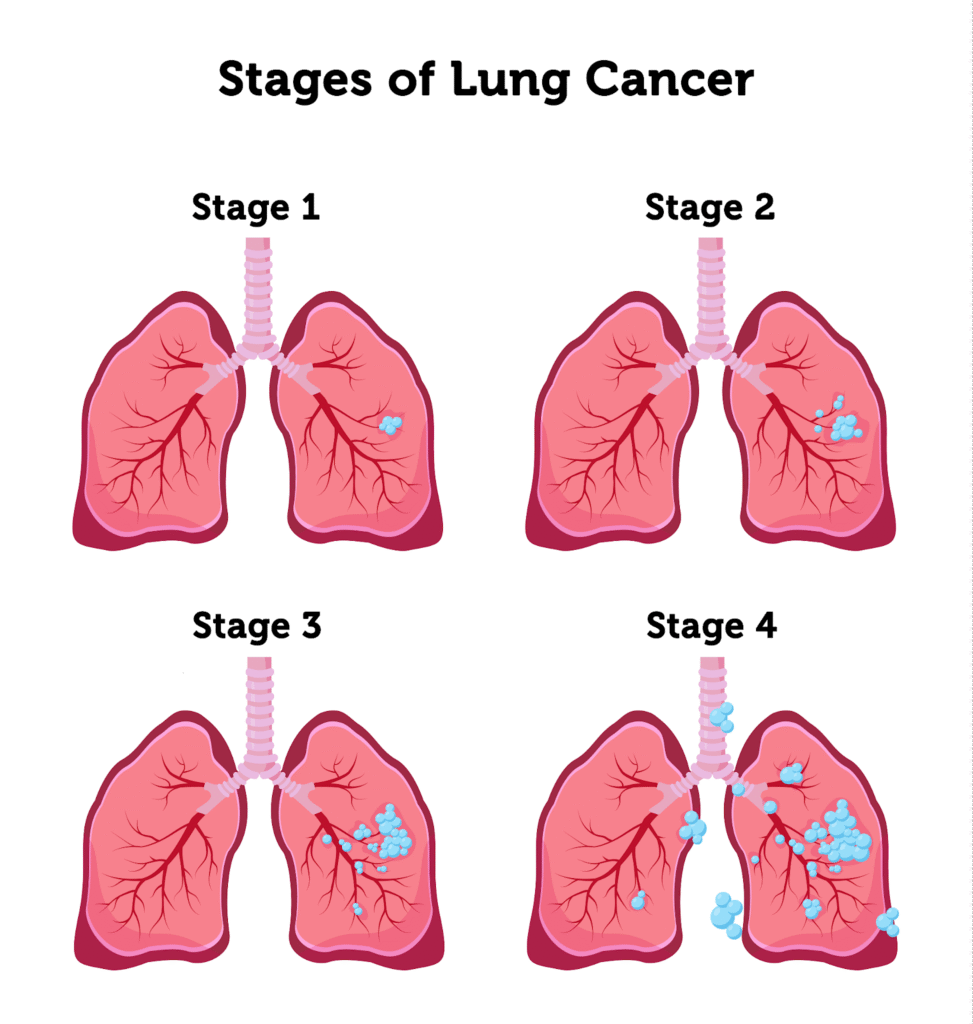
Staging
Lung cancer staging helps doctors understand how far the disease has progressed and guides treatment decisions. Staging is commonly based on the TNM system, which looks at three key factors:
- T (Tumour): The size of the primary tumour and whether it has grown into nearby tissues.
- N (Nodes): Whether the cancer has spread to nearby (draining) lymph nodes.
- M (Metastasis): Whether the cancer has spread more widely to other parts of the body, such as the liver, bones, adrenal glands, or brain.
By combining these factors, doctors classify lung cancer into stages, from early (localized) to advanced (metastatic), which helps determine the most effective treatment plan.
Surgery
if you have early stage non-small cell lung cancer you will most likely have surgery to remove the tumour. There are three main types of surgery:
- lobectomy – a lobe is removed
- wedge resection – part of the lobe is removed
- pneumonectomy – a whole lung is removed.
Surgery is rarely used to treat small cell lung cancer. The main treatment for small cell lung cancer is chemotherapy. In addition, radiation therapy can be used to treat stages I-III small cell lung cancer.
Radiation therapy (radiotherapy)
Radiation therapy (also known as radiotherapy) uses x-rays to kill or damage cancer cells and may be offered alone or in combination with surgery or chemotherapy. Radiation therapy can be used to treat locally advanced (stage III) non-small cell lung cancer. You may have radiation therapy for early stage lung cancer if surgery is not an option. Radiotherapy may also be used after surgery or as a palliative treatment.
Thermal ablation
If surgery or radiation therapy are not suitable, you may be offered ablation treatment for localised, stage I non-small cell lung cancer. You will have needles inserted into the cancer to destroy cancer cells by heating them.
Chemotherapy
Chemotherapy uses anti-cancer drugs to destroy cancer cells. It can be used to treat both small cell and non-small cell lung cancer. Chemotherapy may be used before surgery to shrink a tumour. It may be used before or in conjunction with radiation therapy to improve its effectiveness, before surgery to shrink the cancer, or after surgery to reduce the risk of cancer coming back.
Immunotherapy
Immunotherapy uses specific drugs to stimulate the body’s immune system and can be used to treat some forms of non-small cell lung cancer.
Targeted therapy
Targeted therapy or personalized medicine targets specific mutations in cancer cells. Targeted therapy is generally used for advanced non-small cell lung cancer or if the cancer has returned.
Palliative care
Palliative care seeks to improve quality of life by reducing cancer symptoms without aiming to cure the disease. Palliative treatment can be used at any stage of advanced lung cancer to assist with managing symptoms such as pain and nausea as well as slow the spread of the cancer.
Treatment Team
Depending on your treatment, your treatment team may consist of a number of different health professionals, such as:
- GP (General Practitioner) – looks after your general health and works with your specialists to coordinate treatment.
- Respiratory physician – investigates symptoms, is involved in diagnosis and determines initial treatment options.
- Thoracic (chest) surgeon – diagnoses and performs surgery for cancer and other diseases of the lungs and chest.
- Radiation oncologist – prescribes and coordinates radiation therapy treatment.
- Medical oncologist – prescribes and coordinates the course of chemotherapy.
- Cancer nurse – assists with treatment and provides information and support throughout your treatment.
- Dietitian – recommends an eating plan to follow while you are in treatment and recovery.
- Speech pathologist – helps with swallowing and communication difficulties during and after treatment.
- Other allied health professionals – such as social workers, pharmacists, and counsellors
A personalized treatment plan is usually developed by a healthcare team to achieve the best possible results.
Diagnosis of lung cancer
You may have a number of tests to determine if you have lung cancer.
Chest x-ray
An x-ray can show larger tumours (more than 1cm wide).
CT scan
A computerised tomography (CT) scan uses x-ray beams to take pictures inside your body and create a cross-sectional image. A CT scan is able to detect smaller tumours as well as providing information about the tumour and lymph nodes.
PET scan
A positron emission tomography (PET) scan is used to stage lung cancer after a diagnosis.
Lung function test
You may have a lung function test known as spirometry which checks how well your lungs are working.
Biopsy
A small sample of tissue will be taken if a tumour is suspected after a CT scan or x-ray. There are different types of biopsy including a bronchoscopy, CT-guided core biopsy and endobronchial ultrasound.
Sputum cytology
The sputum (mucus) from your lungs will be examined under a microscope to check for abnormal cells.
After a diagnosis of lung cancer
After finding out you have lung cancer you may feel shocked, upset, anxious or confused. These are normal responses. For most it will be a difficult time, however some people manage to continue with their normal daily activities.
Talk about your treatment options with your doctor, family and friends. Seek as much information as you need. It is up to you how involved you want to be in decisions about your treatment.
Prevention
While not all cases can be prevented, certain steps can greatly reduce the risk of lung cancer:
- Don’t smoke: Quitting smoking is the most effective way to lower your risk. If you smoke, seek support to quit.
- Avoid secondhand smoke: Limit exposure to smoke from others and encourage a smoke-free environment.
- Test your home for radon: This naturally occurring radioactive gas can increase lung cancer risk if present in high levels.
- Protect yourself at work: Follow safety measures to avoid exposure to asbestos and other harmful chemicals.
- Eat a healthy diet: Focus on fruits, vegetables, and whole grains for their protective antioxidants.
- Exercise regularly: Physical activity improves overall health and may help reduce cancer risk.

